If you’ve ever had surgery, or simply had a tooth out, then you’ll know popping a couple of Ibuprofen just isn’t going to cut it, you want to be numb, or even better, unconscious… Enter the anaesthetists.
Medics have been using anaesthetic drugs for over 150 years and they have plenty of clinical evidence that they work extremely well. But how does anaesthetic actually work? And how much to we understand about what we experience when we lose consciousness?
During anaesthesia for major surgery, drugs prevent you being aware of painful sensations. Doctors often conduct minor surgery, and other procedures, under local anaesthesia, and use sedative drugs to calm you.
General anaesthetics and sedatives alter your state of consciousness. Anaesthetists commonly give them in combination with powerful painkillers to make sure your surgery is as painless as possible.
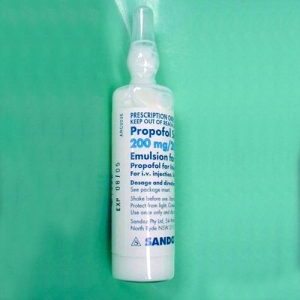 Today general anaesthesia often begins with an injected dose of the drug propofol. Researchers know a good deal about how this drug works on a cellular level.
Today general anaesthesia often begins with an injected dose of the drug propofol. Researchers know a good deal about how this drug works on a cellular level.
‘Our cell research showed us that propofol influences receptors on certain nerve cells. These nerves normally respond to a chemical messenger called GABA that stops them sending signals. Propofol mimics the effects of GABA and inhibits nerve signals.’ says Jeffery L Barker from the Laboratory of Neurophysiology, part of the NINDS institute in Bethseda, Maryland
Propofol is only one of many different types of anaesthetic drugs. Each type appears to affect different sets of receptors in the brain, but they all make you lose consciousness.
Because some anaesthetic drugs influence different kinds of neuron compared with others, their precise effects on the brain may be very different.
Brain research tools can show which areas of the brain are affected by different anaesthetics. With fMRI (functional magnetic resonance imaging), for example, a scanner shows brain activity in 3D. On the other hand, when an EEG (electroencephalogram) is recorded, non-invasive electrodes are stuck onto your scalp to measure electrical activity on the brain surface.
EEGs and fMRIs can measure brain activity during different levels of consciousness: awake, asleep and even anaesthetised.
So what can today’s brain imaging technologies tell us about how anaesthetics work?
Steven Laureys leads the Coma Science Group at the University of Liège in Belgium. In an experiment he anaesthetised patients and scanned their brains.
‘Even when volunteers were unconscious, small “islands” in the sensory cortex of their brains showed activity in response to external stimuli,’ says Steven. ‘But this activity did not spread through the brain to areas that control behaviour and memory. This means that although your brain responds to sensations while you’re unconscious, memories don’t form as they would normally.’
Most people seem to have to no memories of sensations during surgery. But Jackie Andrade, Professor of Psychology at Plymouth University, has demonstrated that we’re able to form partial, ‘implicit’, memories under anaesthesia.

‘We tested patients by having them listen to certain words during surgery under general anaesthesia. When they came around, we found that the patients responded differently to words we had played while they were “unconscious” than to other words.’
There are two groups of patients with explicit memories of surgery: those who can remember pain and those who can’t. If you remember pain, you are much more likely to develop post-traumatic stress. But Jackie thinks that implicit memories may also affect you.
‘Although you’re not aware of these memories at all, they could affect recovery times after surgery and cause psychological stress.’
‘Implicit memory could be used to benefit patients undergoing surgery. Encouraging and positive comments made in the operating theatre could be used to reassure patients and reduce anxiety, even while they’re unconscious.’
So how can research improve future anaesthesia?… Do we just need better drugs?
Consultant anaesthetist Andrew Morley from St Thomas’ Hospital in London thinks new drugs are not the top priority.
 ‘Patients having surgery under anaesthesia in future will benefit more from small changes in all aspects of the process than from a single “miracle” anaesthetic drug,’ says Andrew.
‘Patients having surgery under anaesthesia in future will benefit more from small changes in all aspects of the process than from a single “miracle” anaesthetic drug,’ says Andrew.
‘Even if we don’t know exactly how they work, today’s general anaesthetics are highly effective. Before surgery, I consider both patient and planned operation in deciding the best combination of drugs and techniques. I aim to provide good operating conditions for the surgeon, minimising side effects and getting the best possible outcome for each patient. It’s a bespoke business.’
Could new technology be the answer?
The fEITER is a portable imaging technology that has successfully recorded 3D images from anaesthetised brains as they lose consciousness.
Brian Pollard, who developed fEITER the University of Manchester, explains:
‘These images gave us confirmation that losing consciousness involves changes in electrical activity deep inside the brain. Finding out about the process of anesthesia and sedation can help us monitor brain function in the operating theatre, and reduce the risk of painful awareness during surgery.’
But are high tech monitors alone enough to improve anaesthesia?
Emery Brown’s work at the Department of Anaesthesia, Massachusetts General Hospital and at the Department of Brain and Cognitive Sciences, MIT spans two disciplines: anaesthesia and neuroscience. He believes electroencephalogram (EEG) recordings allow anaesthetists to see when someone is unconscious and to understand how anaesthetic drugs create altered states.

‘Different drugs produce signatures that are readily interpretable using EEG. I can see signatures which indicate that the brain is unable to process information, which would mean that you are unconscious. In the future, we may be able to identify the brain circuits for consciousness and pain, and treat them directly using targeted drugs delivered to these circuits.’
Emery believes painful awareness can be prevented by training anaesthetists in neuroscience so they can interpret how EEG readings relate to underlying brain states.
‘The true culprit in cases of awareness is anaesthetists not being able to tell when a patient is unconscious. They often rely on brain activity monitors that are grossly simplified.
‘I can understand detailed raw EEG readings. If you came to me and told me you were afraid you were going to be aware during surgery, I would tell you that I can keep it from happening by keeping an eye on your EEG.’
It is clear to see experts are approaching this issue from all sides. But in the end it may all come down to the skilled experts in the operating theatre…
Andrew Morley explains, ‘Preventing painful awareness in surgery is not only about technology and understanding the brain.’ says Andrew Morley. ‘For decades, scientists and clinicians have tried to use the EEG – raw and otherwise – to distinguish conscious from unconscious patients reliably. No-one’s got it quite right yet – awareness still happens.’
‘Improving anaesthesia is also a matter of improving vigilance in the operating theatre and reducing the likelihood of human error. The Royal College of Anaesthetists and Association of Anaesthetists of Great Britain and Ireland are gathering information on real cases of accidental awareness during general anaesthesia. The results may help us progress towards a better practice and healthier patients.’